Press Releases
-
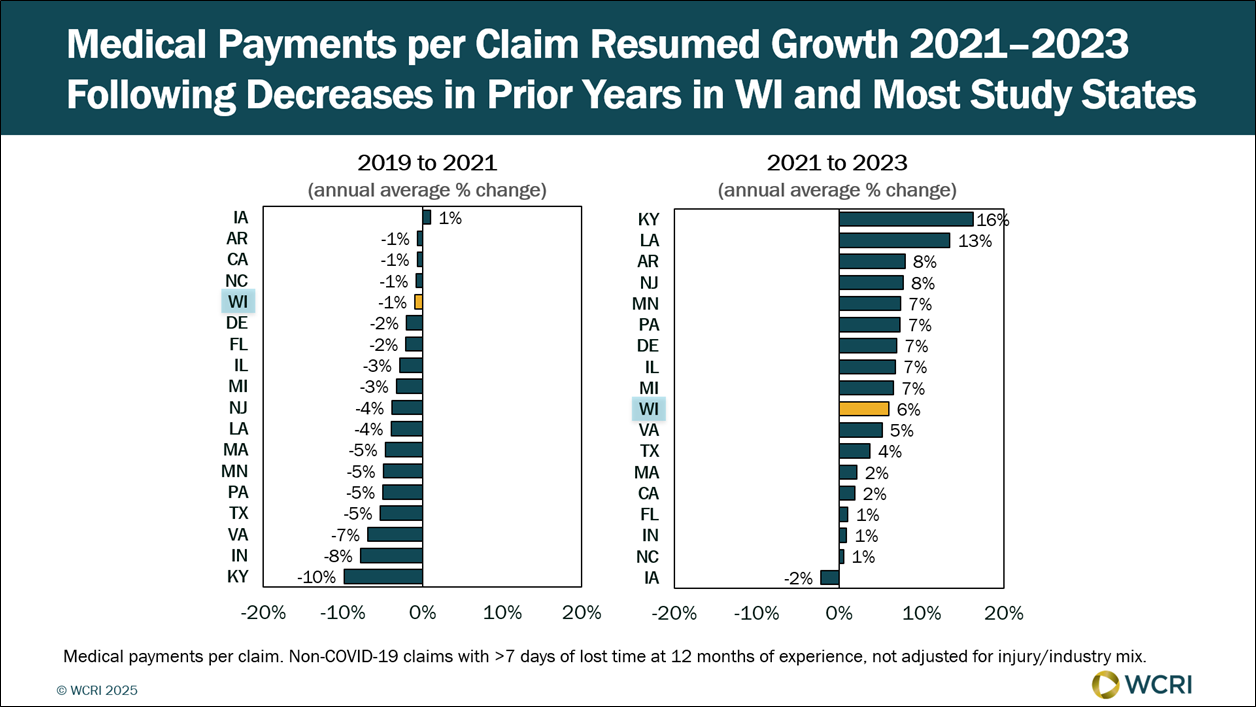

WCRI: Medical Costs per Claim in Wisconsin Grew 6% per Year
Waltham, MA, Nov. 13, 2025 – Medical payments per claim in Wisconsin grew 6% per year from 2021 to 2023 after years of modest changes, according…
-


Insurance and Risk Expert Dr. Bob Hartwig to Keynote 2026 WCRI Conference
Waltham, MA, Nov. 12, 2025—The Workers Compensation Research Institute (WCRI) announced today that Dr. Bob Hartwig will deliver the keynote…
-
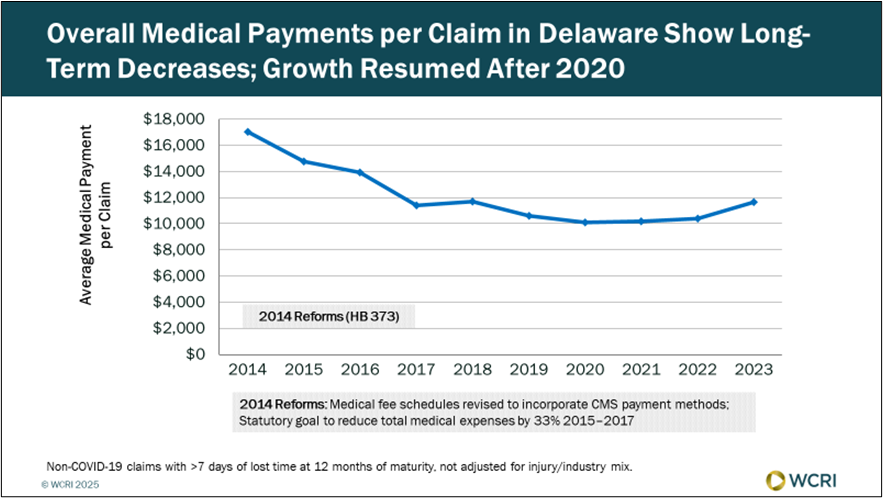

WCRI: Medical Costs per Claim in Delaware Grew 7% per Year
Nov. 6, 2025 – Medical payments per claim in Delaware grew 7% per year between 2021 and 2023, driven by price increases in professional and…
-


WCRI Webinar: Advanced Practitioners and Workers’ Compensation Claim Outcomes
Waltham, MA, November 4, 2025 – The Workers Compensation Research Institute (WCRI) will host a free 40-minute webinar on Thursday, November 20,…
-
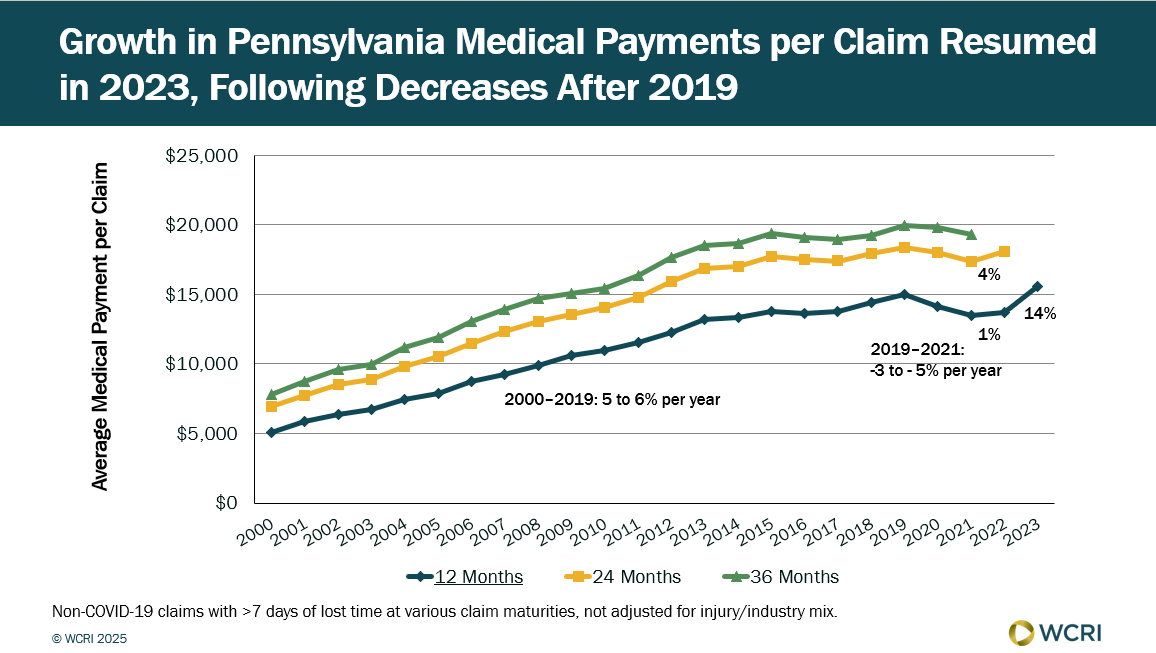

WCRI: Medical Costs per Claim in Pennsylvania Rose 14% in 2023, Following Decreases in Past Years
Waltham, MA, October 23, 2025 – Medical payments per claim for injured workers in Pennsylvania rose 14% in 2023, following relatively stable or…
-
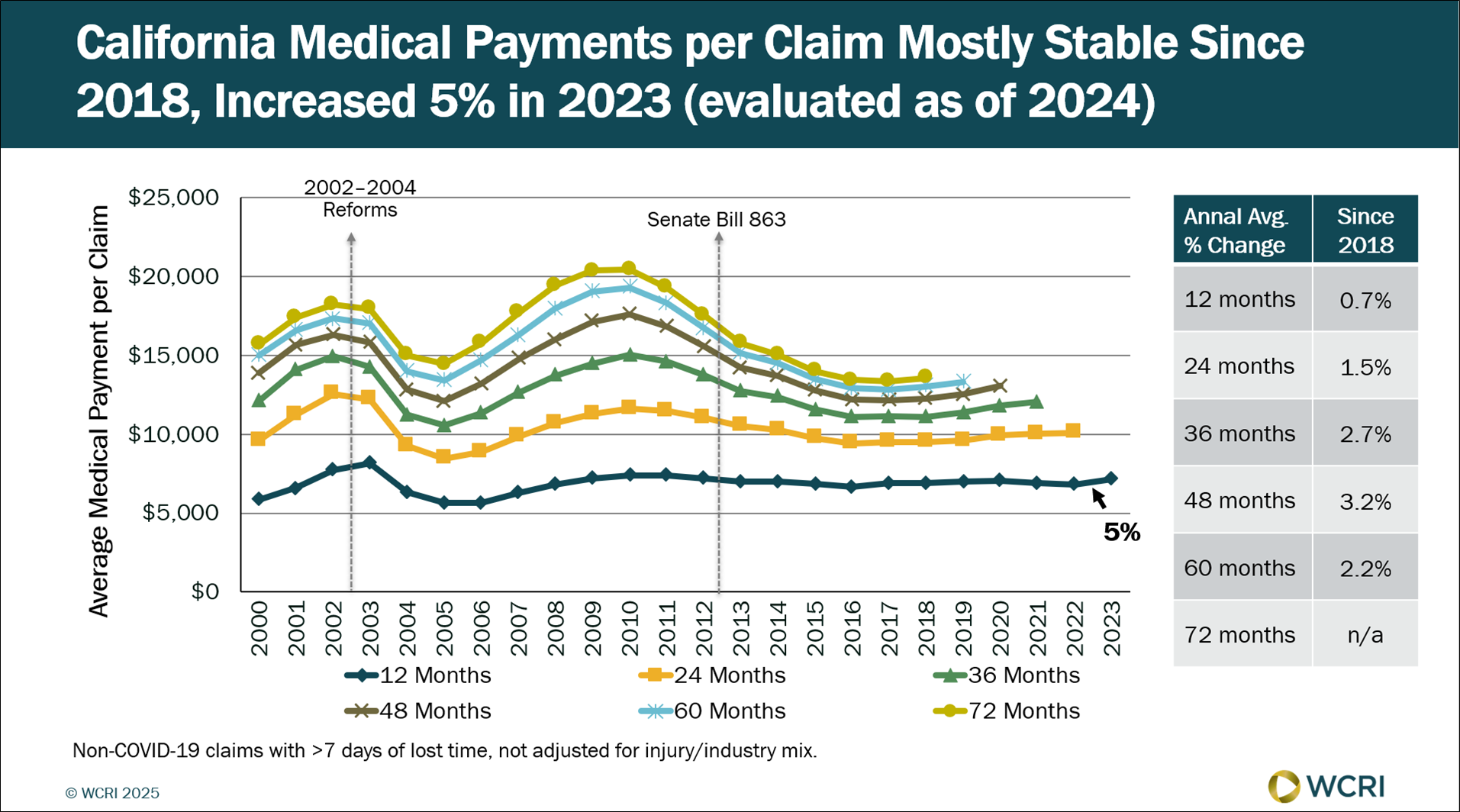

WCRI: Medical Costs per Claim in California Rose 5%
Waltham, MA, October 16, 2025 – After years of stable payments, medical costs per claim for injured workers in California rose 5% as of 2024,…
-


Webinar: Impact of California’s Heat Standard on Workers’ Compensation Outcomes
Waltham, MA, October 15, 2025 – The Workers Compensation Research Institute (WCRI) announced a 30-minute webinar scheduled for Thursday, October…
-
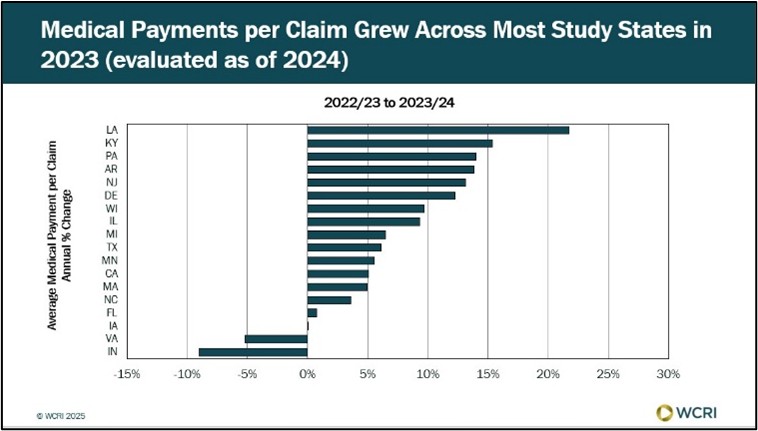

Medical Costs per Claim Rose 5–12% Across Majority of States
Waltham, MA, October 9, 2025 — After a period of relative stability post-COVID, new studies from the Workers Compensation Research Institute…
-


WCRI: California Heat Standard Reduced Work Injuries by Over 15% on Hot Days in High-Exposure Industries
Waltham, MA – Sept. 30, 2025 — As more states adopt heat safety standards, a new study from the Workers Compensation Research Institute (WCRI)…
-

Role of Psychosocial Factors on Recovery from Knee and Shoulder Pain
Behavioral health is increasingly recognized as a key factor in workers’ compensation recovery. Psychosocial risks—like fear of movement, poor…
-


Webinar: Highlights of Florida’s Workers’ Compensation System
Waltham, MA, September 4, 2025― The Workers Compensation Research Institute (WCRI) will host a free, 45-minute webinar on Thursday, September 25,…
-

Back and Shoulder Injuries with a $65K+ Price Tag: New WCRI Study Examines the Causes
Waltham, MA – August 7, 2025 — A new study from the Workers Compensation Research Institute (WCRI) examines the key factors associated with…
-


Does Care Started by Advanced Practitioners Result in Different Outcomes?
Waltham, MA – July 24, 2025 – As the shortage of primary care physicians grows, more injured workers are receiving initial care from advanced…
-

Study Highlights Specific Factors Driving High-Cost Rotator Cuff Disorder Claims
Waltham, MA – July 8, 2025 – A new study by the Workers Compensation Research Institute (WCRI) identifies detailed factors associated with…
-


Impact of Inflation on Workers’ Compensation Medical Payments from 2020 to 2025
Waltham, MA, June 30, 2025 – A new study from the Workers Compensation Research Institute (WCRI) sheds light on how the high-inflation period of…
-


New WCRI Study Explores Promises and Challenges of Artificial Intelligence in Workers’ Compensation
Waltham, MA, June 25, 2025 — A new study from the Workers Compensation Research Institute (WCRI) examines how stakeholders view the promises and…
-


Striking the Balance: WCRI Study Reveals Key Decisions in Workers’ Comp Fee Schedules
Waltham, MA, June 20, 2025 – As policymakers seek to implement or revise price controls in their state workers’ compensation systems through…
-
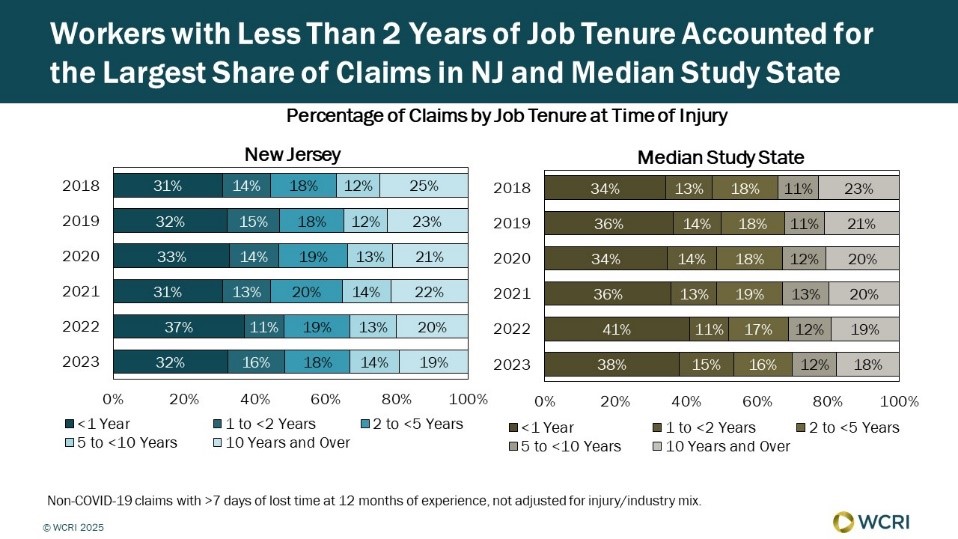

WCRI: Growth of Short-Tenure Workers as Share of Claims in New Jersey Echoes National Trend
Waltham, MA, June 10, 2025 – Short-tenure workers, meaning those with less than two years of job tenure, continued to account for the largest…
-


Webinar: Heat-Related Illnesses in the Workplace
Waltham, MA, June 5, 2025 — With summer approaching, the Workers Compensation Research Institute (WCRI) is hosting a free, 30-minute webinar on…
-


Hospital Outpatient Payments Grew Faster in States with Charge-Based or No Fee Schedules
Waltham, MA, May 29, 2025 – As policymakers nationwide focus on the rising costs of health care, a new study from the Workers Compensation…
-
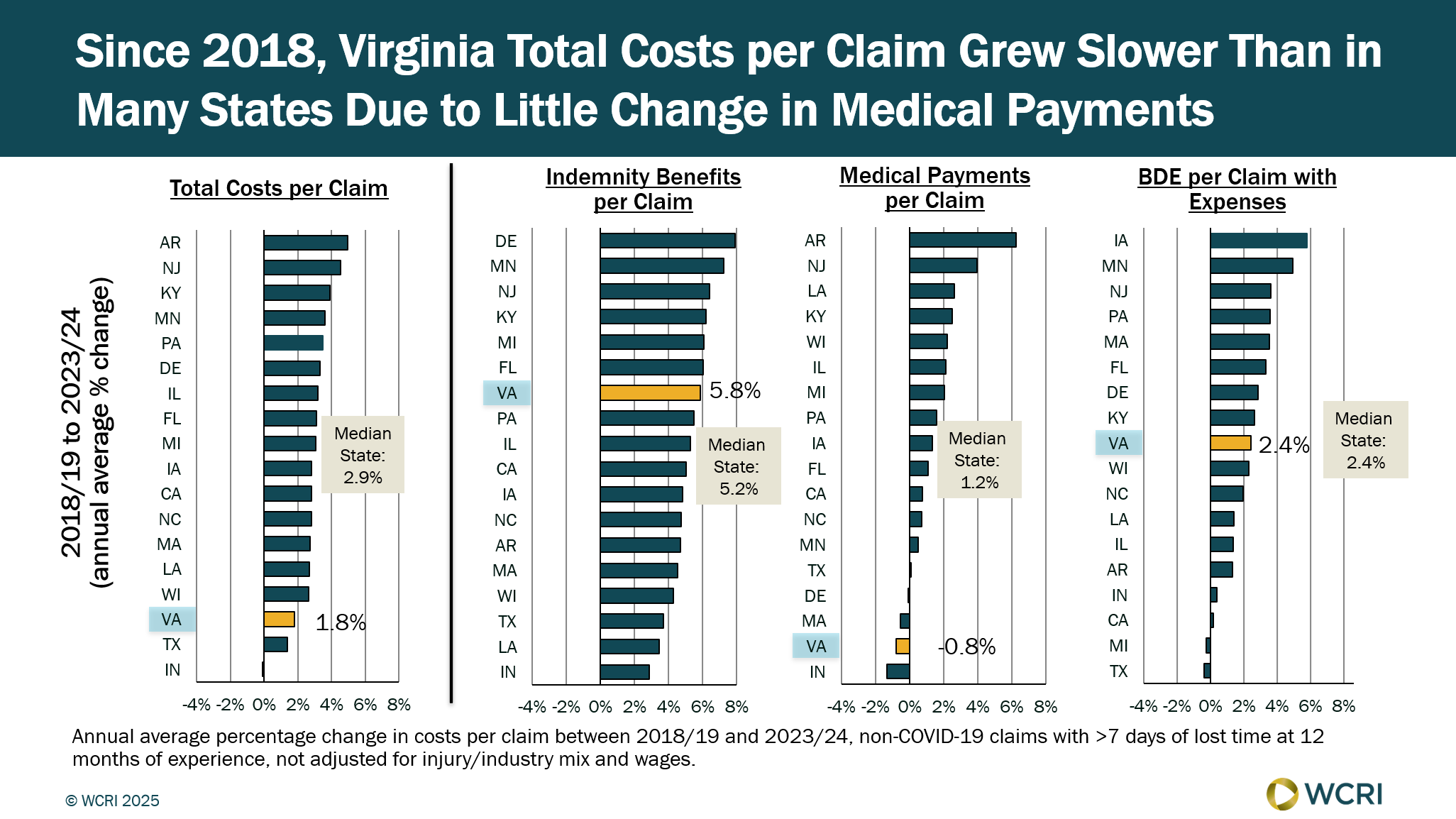

WCRI: Virginia Workers’ Compensation Claims Costs Grew Slower Than Most States
Waltham, MA, May 27, 2025 – A recent study from the Workers Compensation Research Institute (WCRI) found that total costs per workers’…
-
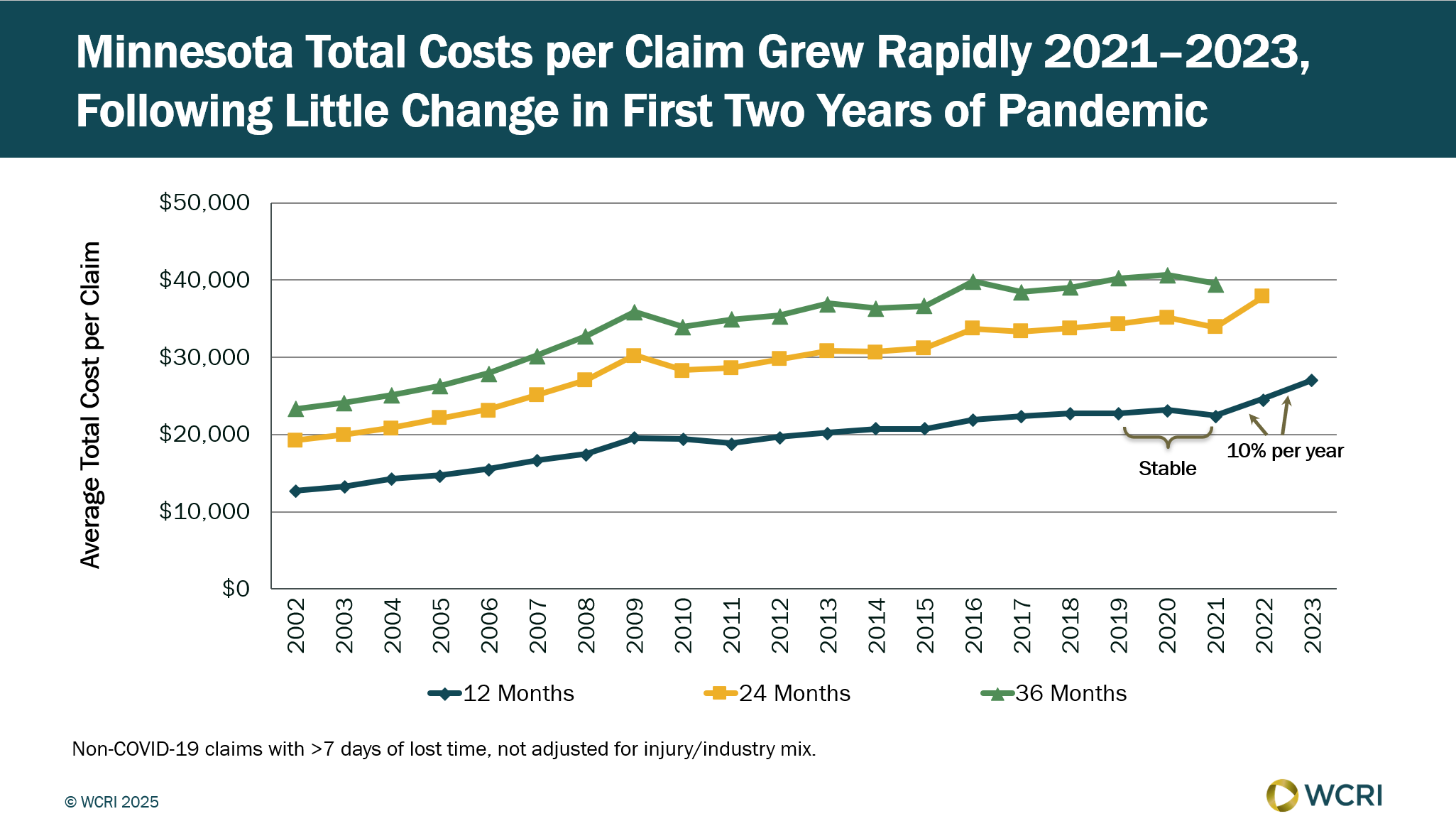

WCRI: Minnesota Seeing Rapid Growth in Total Costs per Workers’ Compensation Claim
Waltham, MA, May 22, 2025 – Workers’ compensation costs per claim in Minnesota rose about 10 percent annually from 2021 to 2023, following…
-
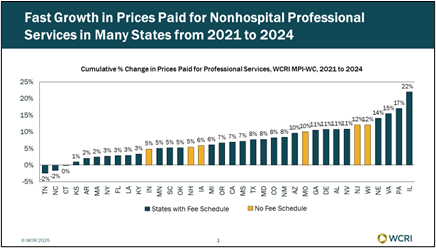

General Inflation Having an Impact on Faster Growth in Workers’ Compensation Medical Prices
Waltham, MA, May 20, 2025 —The Workers Compensation Research Institute (WCRI) has released the 2025 edition of its annual study, WCRI Medical…
-
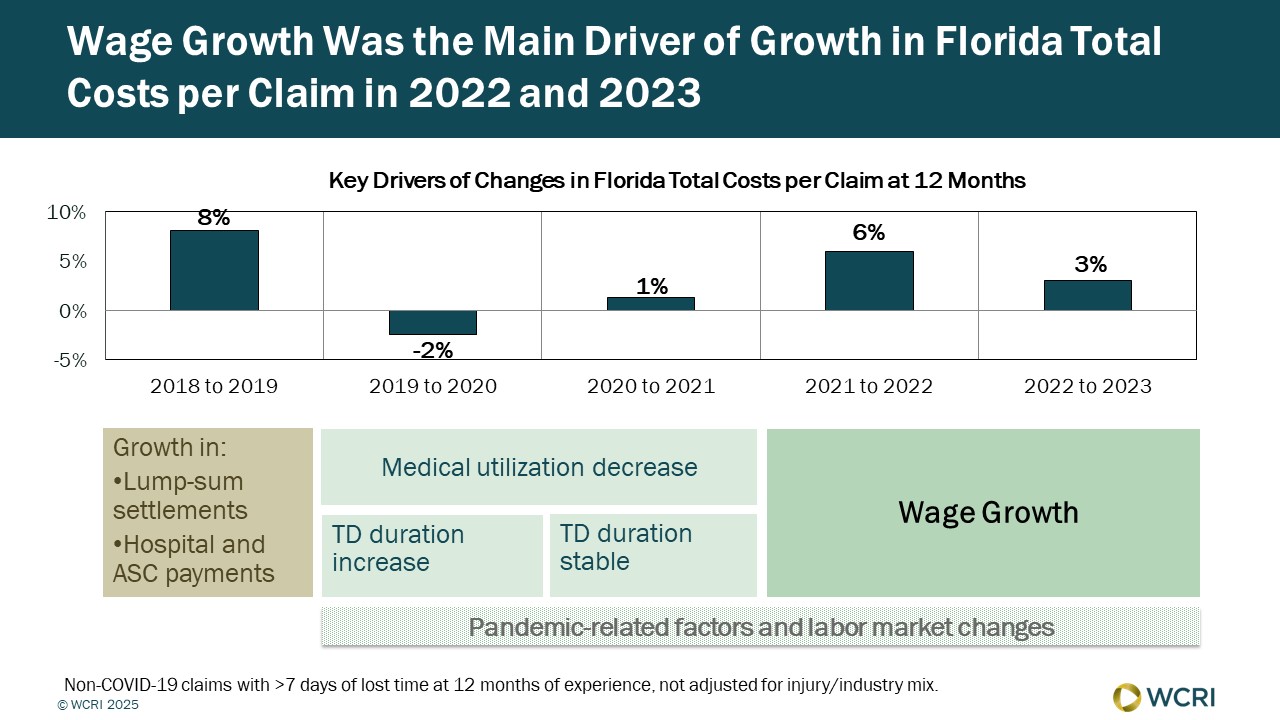

WCRI: Recent Trends in Florida Costs per Workers’ Compensation Claim Highly Influenced by Wages
Waltham, MA, May 13, 2025 – The recent changes in overall costs per claim in 2022 and 2023 in Florida were largely due to wage growth, according…
-
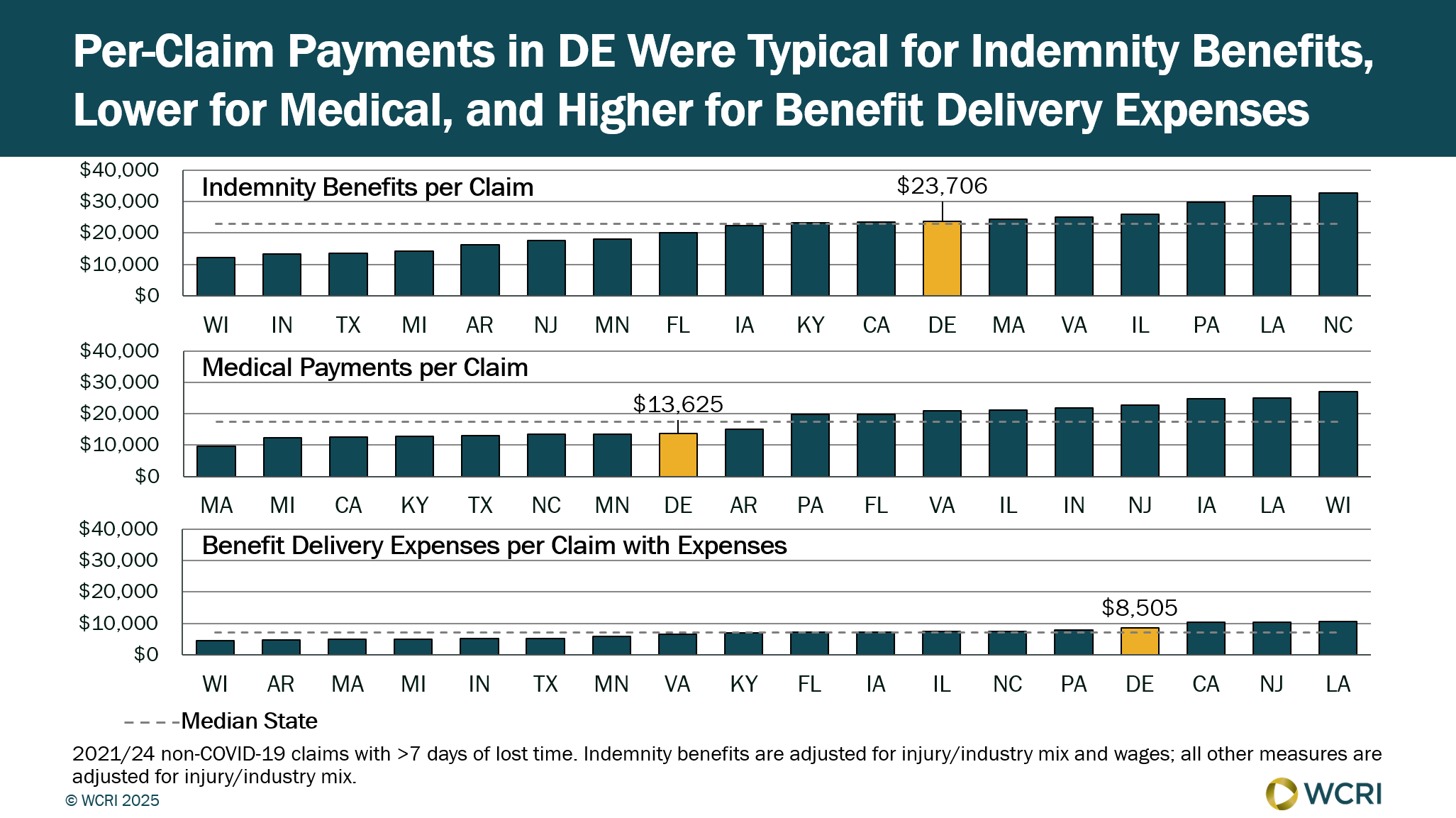

WCRI: Total Cost per Workers’ Compensation Claim in Delaware Remains Stable
Waltham, MA, May 6, 2025 – A new study from the Workers Compensation Research Institute (WCRI) finds that total costs per workers’ compensation…
-


Impact of Recreational Marijuana Laws on Workers’ Compensation Benefits
Waltham, MA, April 30, 2025 – As more states adopt recreational marijuana laws (RMLs), a new study by the Workers Compensation Research Institute…
-
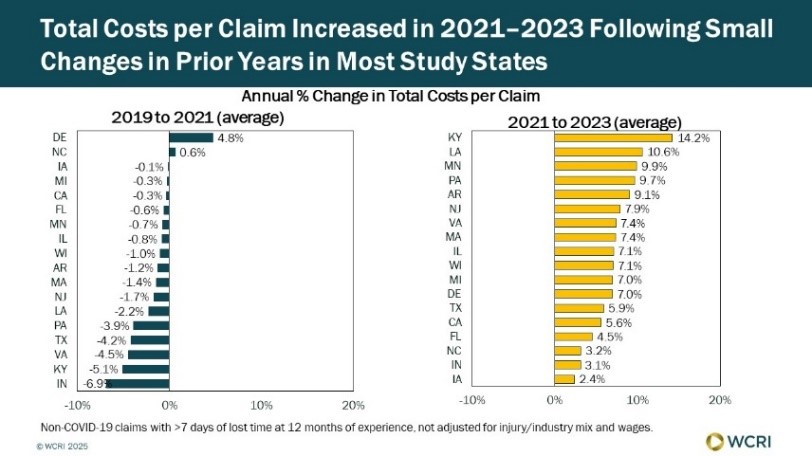

WCRI: Total Costs per Workers’ Compensation Claim Increased Across 18 Study States
Waltham, MA, April 28, 2025―Total costs per workers’ compensation claim rose between 2 and 14 percent annually from 2021 to 2023 across 18…
-

WCRI Report: Comorbidities Increase Claim Costs and Duration of Temporary Disability
Waltham, MA, March 27, 2025 – A new report from the Workers Compensation Research Institute (WCRI) reveals that claims involving degenerative…
-


2025 WCRI Annual Report Now Available
Waltham, MA, March 25, 2025 – The Workers Compensation Research Institute (WCRI) is pleased to announce the release of its 2025 Annual Report,…
-


New Report Compares Workers’ Compensation Laws Across U.S. States and Canada
Waltham, MA, February 27, 2025 – A new report from the Workers Compensation Research Institute (WCRI) and the International Association of…
-


New WCRI Report: COVID-19’s Impact on Medical Utilization by Age and Tenure
Waltham, MA, February 25, 2025 —The Workers Compensation Research Institute (WCRI) has released a new FlashReport exploring how medical…
-
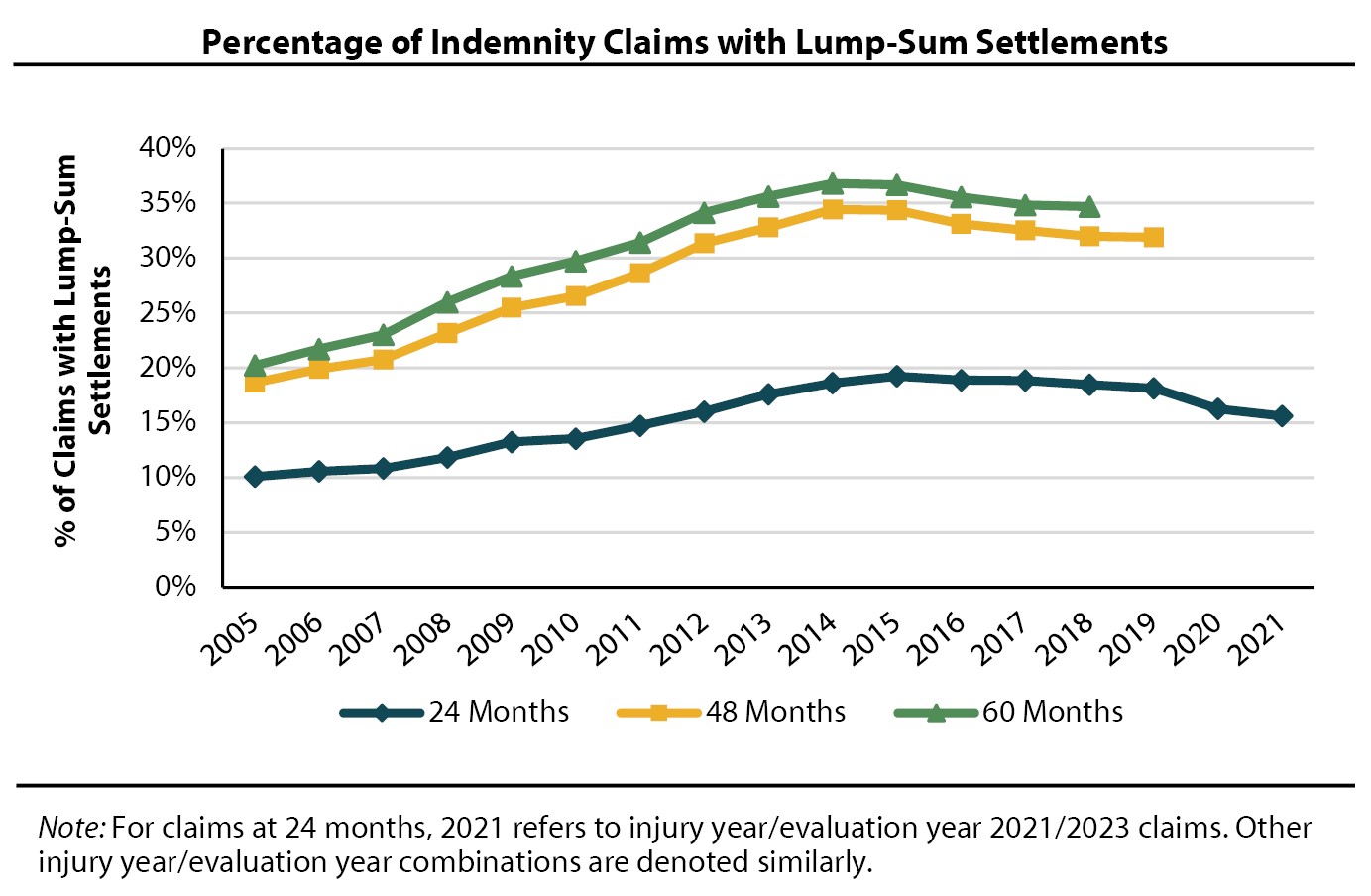

WCRI Report: Lump-Sum Settlements More Frequent in New York Following 2007 Reforms
Waltham, MA, January 30, 2025 — A new report from the Workers Compensation Research Institute (WCRI) revealed a rise in the frequency of lump-sum…
-
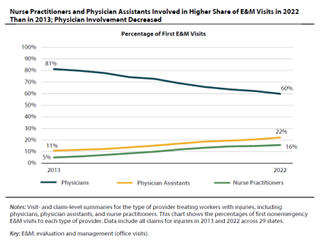

WCRI Examines Impact of Recent Medical Workforce Trends on Injured Workers
Waltham, MA, January 23, 2025 — A new study from the Workers Compensation Research Institute (WCRI) analyzes recent changes in the composition of…
-


UNC Prof. Holmes to Discuss Rural Healthcare Access Threats at 2025 WCRI Conference
Waltham, MA, January 22, 2025 — The Workers Compensation Research Institute (WCRI) is excited to announce that University of North Carolina (UNC)…
-
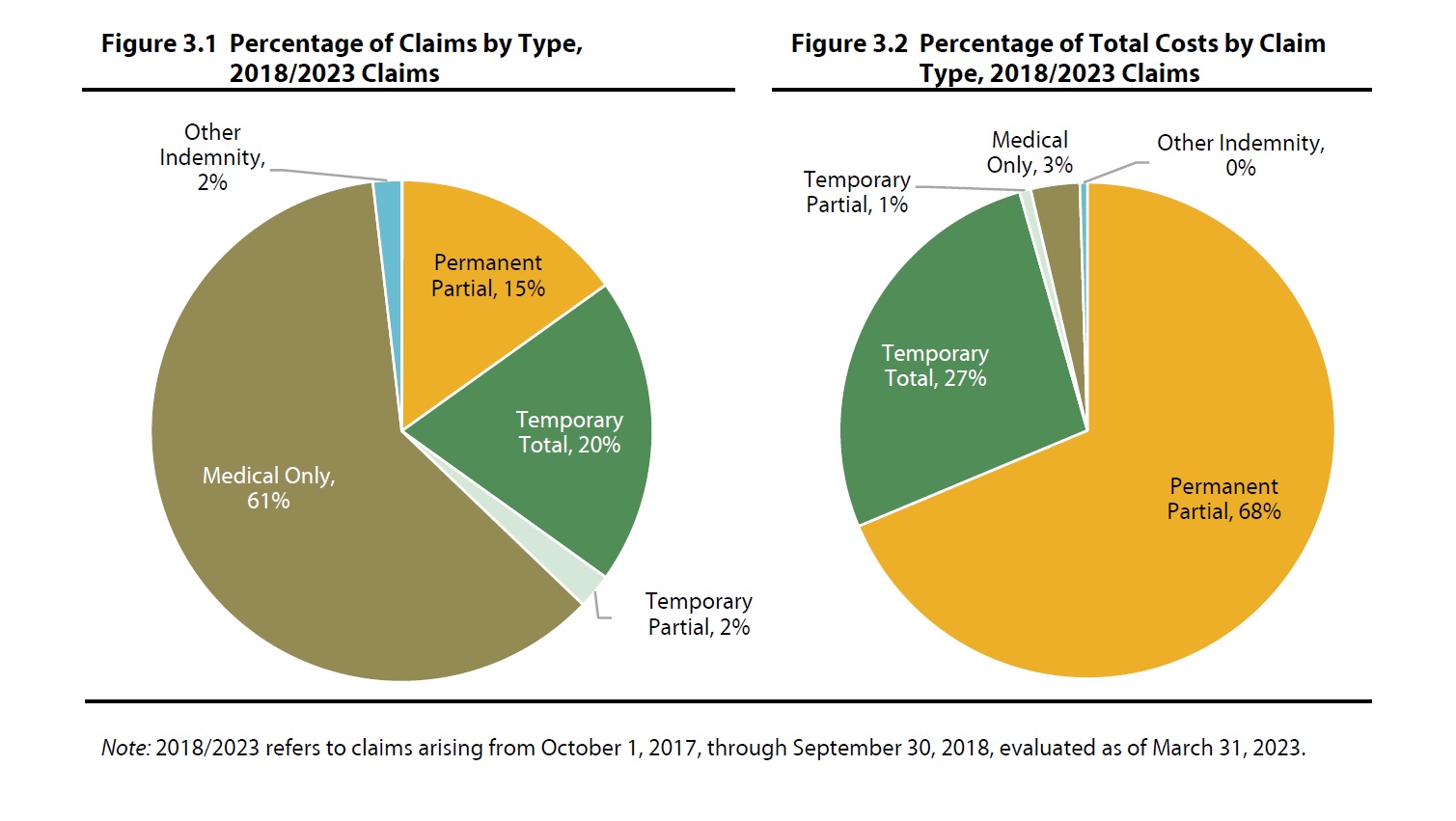

WCRI: Examining the Life Cycle of New York Workers’ Compensation Claims
Waltham, MA, January 16, 2025 — A new study from the Workers Compensation Research Institute (WCRI) offers an in-depth look at workers'…
-
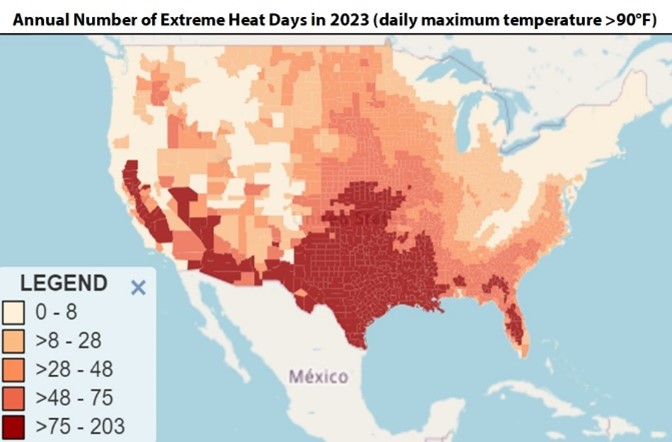

WCRI: Incidence of Heat-Related Illnesses Rises Dramatically at Temperatures Above 90°F
Waltham, MA, Dec. 18, 2024―As the number of heat-related illnesses (HRIs), such as heat exhaustion and heat stroke, continues to rise, a new…
-
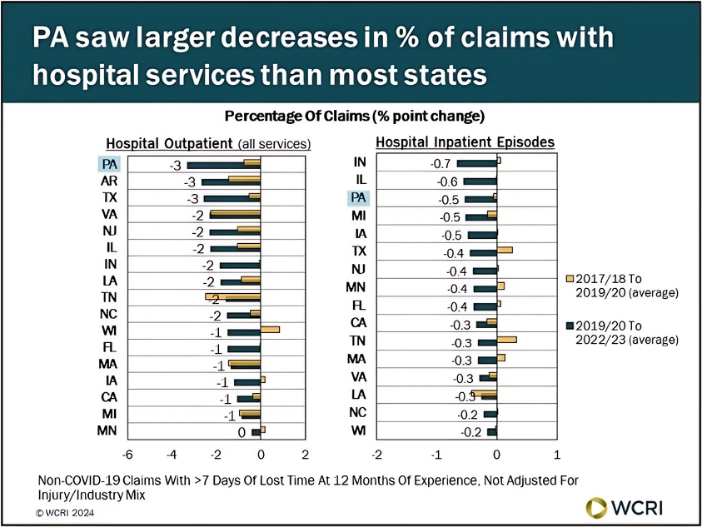

WCRI: Pennsylvania Experiencing Larger Decline in Utilization of Hospital Services Than Many States
Waltham, MA, Nov. 14, 2024 – A recently released study from the Workers Compensation Research Institute (WCRI) found that utilization of hospital…
-
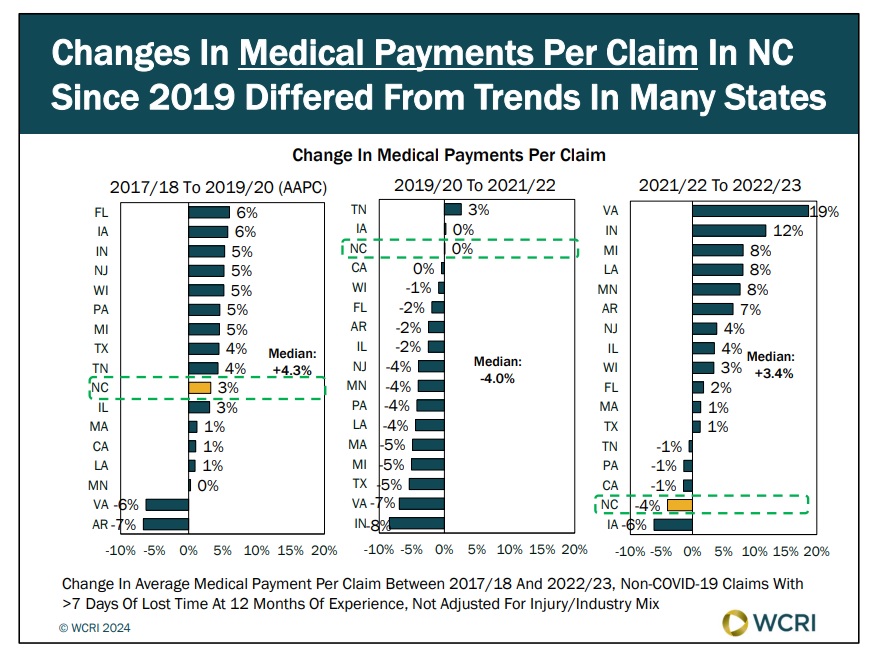

WCRI: North Carolina Medical Payments for Treating Injured Workers Decreased from 2021 to 2022, Unlike in Most States
Waltham, MA, Nov. 7, 2024 – A recent study from the Workers Compensation Research Institute (WCRI) found that medical payments per claim for the…
-
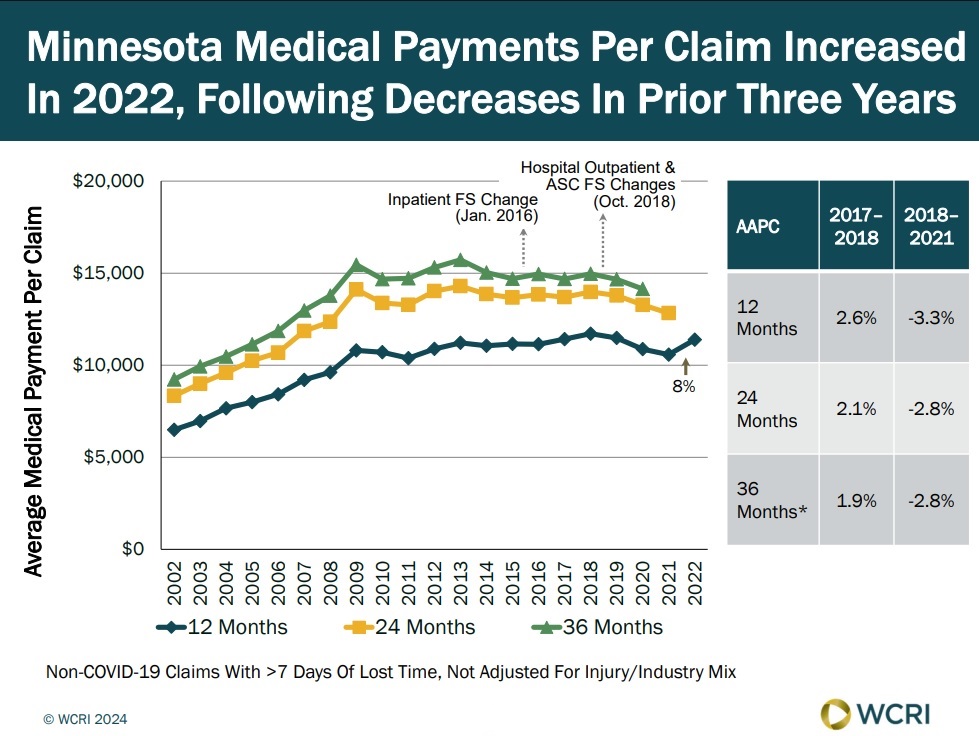

WCRI: Minnesota Workers’ Compensation System Potentially Beginning Rebound from Pandemic Disruptions
Waltham, MA, October 31, 2024 – A recent study from the Workers Compensation Research Institute (WCRI) found that the delivery of medical care to…
-
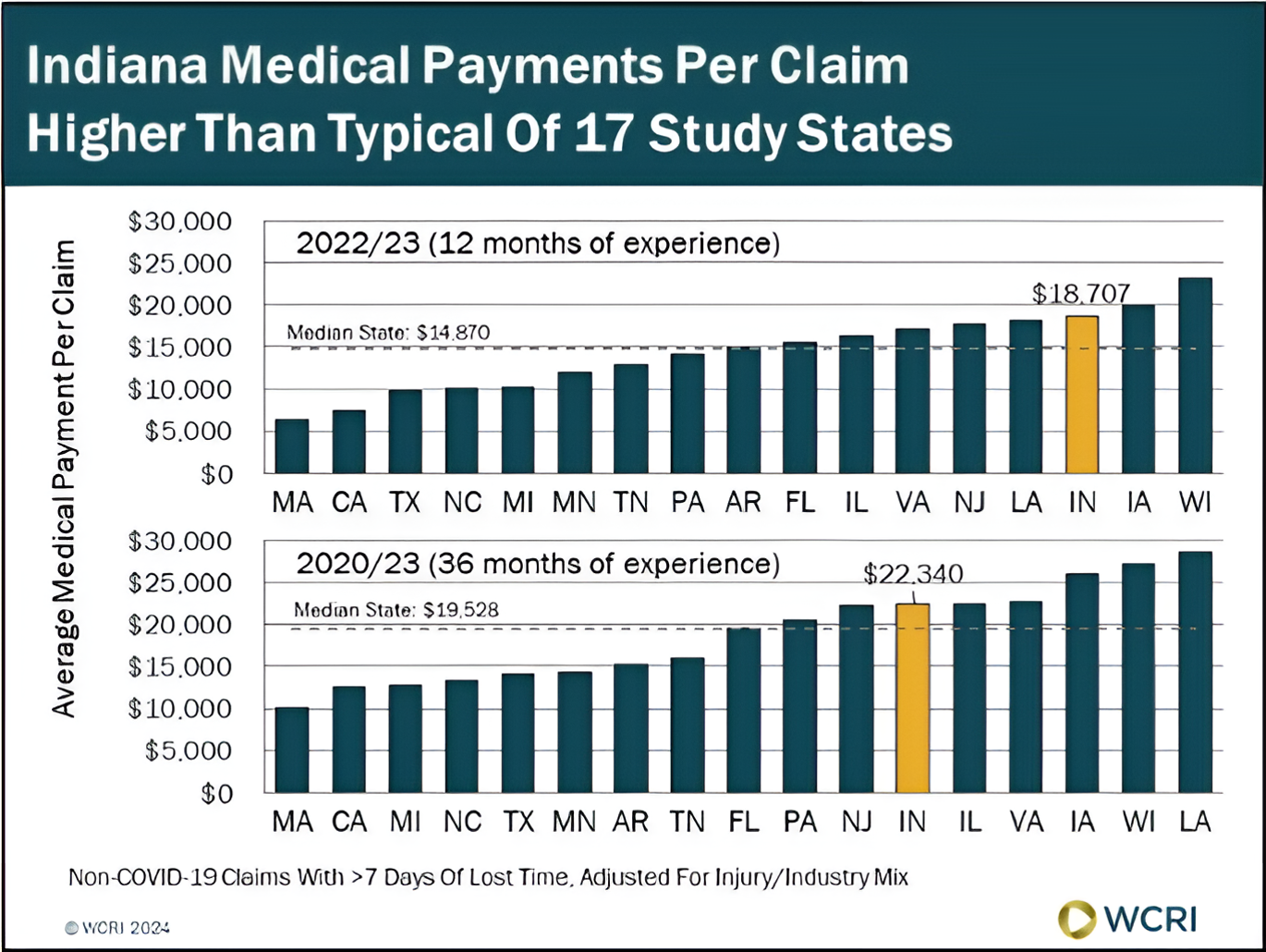

WCRI: Indiana Medical Payments Per Claim Under Workers’ Compensation Higher Than Most States
Waltham, MA, October 24, 2024 – A new study from the Workers Compensation Research Institute (WCRI) found that medical payments per claim for the…
-
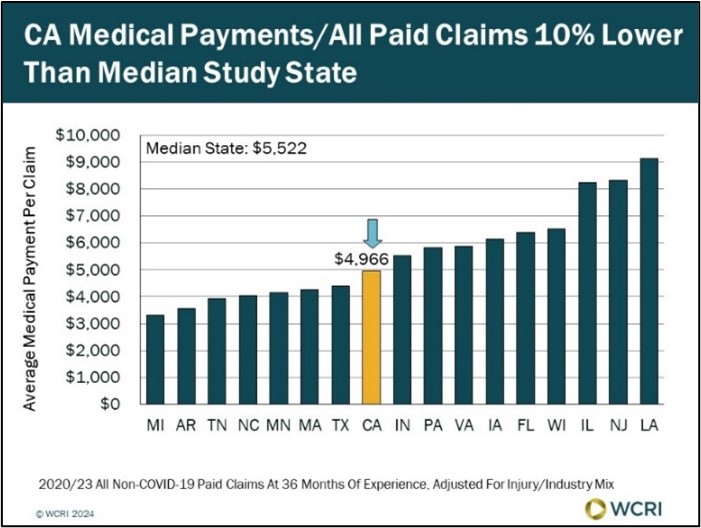

WCRI: Cost of Medical Treatment for Workers Injured in California Near Middle of Study States
Waltham, MA, October 17, 2024—A new study from the Workers Compensation Research Institute (WCRI) found that workers’ compensation medical…
-
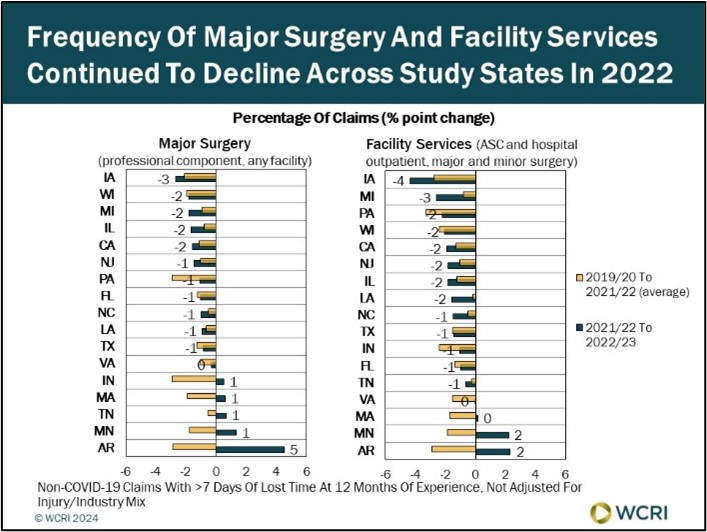

WCRI: Utilization of Medical Care for Workers with Injuries Continues to Decline
Waltham, MA, October 10, 2024 ― A new set of studies from the Workers Compensation Research Institute (WCRI) found that utilization of medical…
-
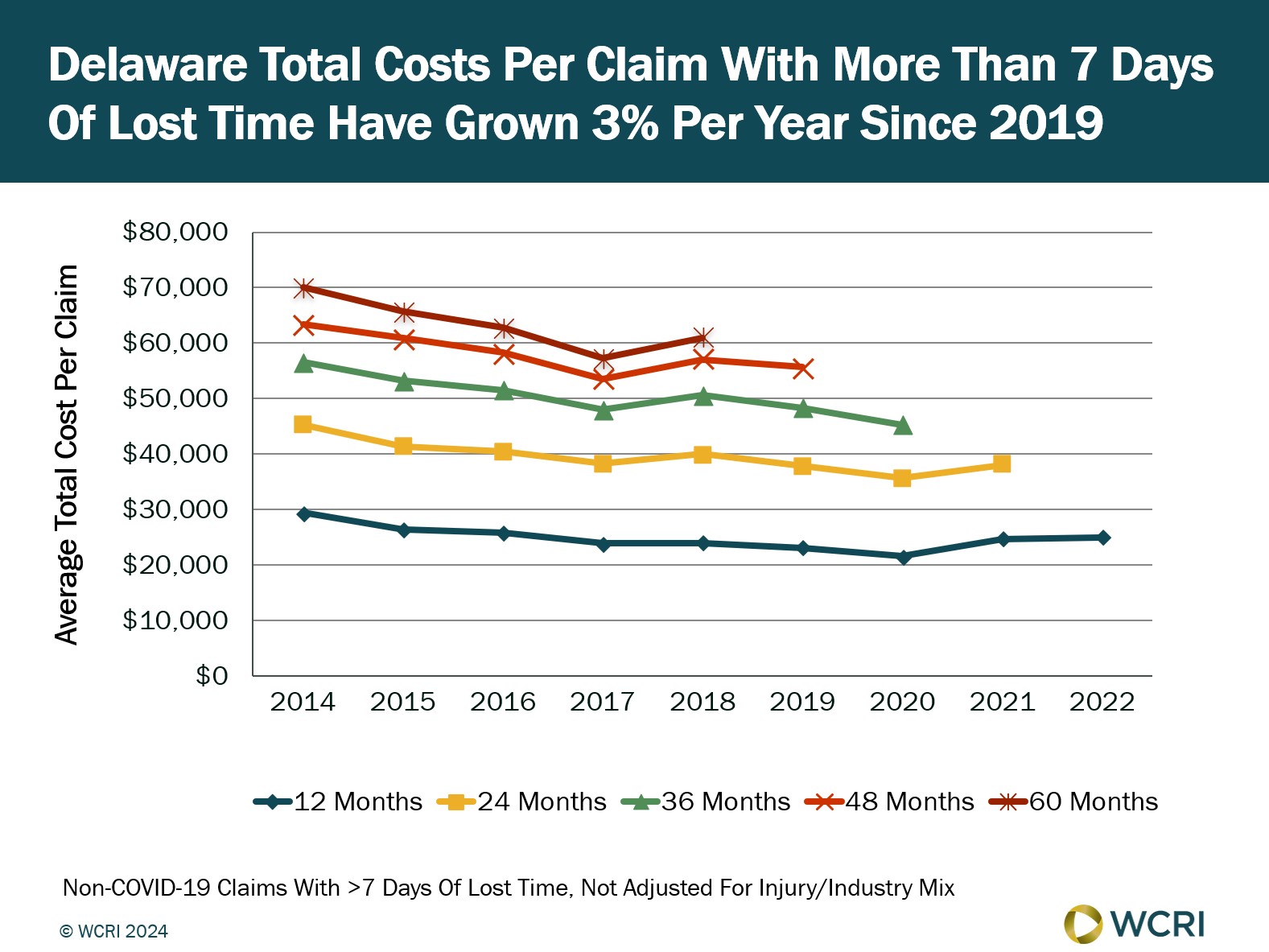

WCRI: Delaware Workers’ Comp Claim Costs Increased 3 Percent Annually (2019–2022)
Waltham, MA, Sept. 30, 2024 — A new study from the Workers Compensation Research Institute (WCRI) shows that the average cost of workers'…
-


WCRI: Impact of Attorney Representation on Workers’ Compensation Payments
Waltham, MA, Sept. 25, 2024―A new study from the Workers Compensation Research Institute (WCRI) examines the effect of attorney involvement on…
-


Registration Now Open for 2025 Annual WCRI Issues & Research Conference
Waltham, MA, Sept. 24, 2024 — The Workers Compensation Research Institute (WCRI) is pleased to announce that registration is now open for its…
-


Webinar: Highlights of the Pennsylvania Workers’ Compensation System
Waltham, MA, Sept. 10, 2024 ― The Workers Compensation Research Institute (WCRI) will hold a free, one-hour webinar on Wednesday, October 2,…
-


WCRI Study Identifies Key Factors Associated with High-Cost Claims in Workers’ Compensation
Waltham, MA, Aug. 8, 2024―Many studies have shown that health care costs are concentrated among a small percentage of individuals with diverse…
-


New Study Highlights Behavioral Health in New York Workers’ Compensation System
Waltham, MA, July 30, 2024―A new study from the Workers Compensation Research Institute (WCRI) examines the prevalence and use of behavioral…
-


WCRI: Half of All Injuries Occurred in the First Two Years of Workers’ Tenure with At-Injury Employer
Waltham, MA, July 18, 2024 ― A new FlashReport from the Workers Compensation Research Institute (WCRI) found that the proportion of injuries…
-


Webinar: Trends in Workers’ Compensation Drug Payments Across States
The Workers Compensation Research Institute (WCRI) will host a 30-minute webinar on Thursday, August 1, 2024, at 2 p.m. ET on its study, Interstate…
-
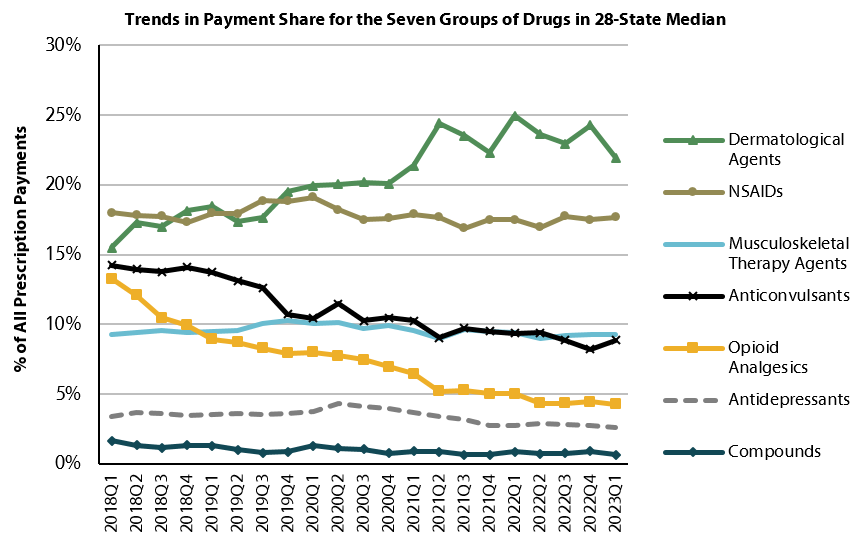

WCRI: Dermatological Agents and NSAIDs Continue to Be Top Cost Drivers in Workers’ Compensation
Waltham, MA, June 20, 2024 ― The latest edition of the Workers Compensation Research Institute (WCRI) drug trends report finds that while…
-


WCRI: Medical Fee Schedules Play Big Role in Shaping Price Changes During Inflationary Period in State Workers’ Compensation Systems
Waltham, MA, June 13, 2024—In recent years, inflation in the workers’ compensation system has been a concern, as inflation in the overall…
-
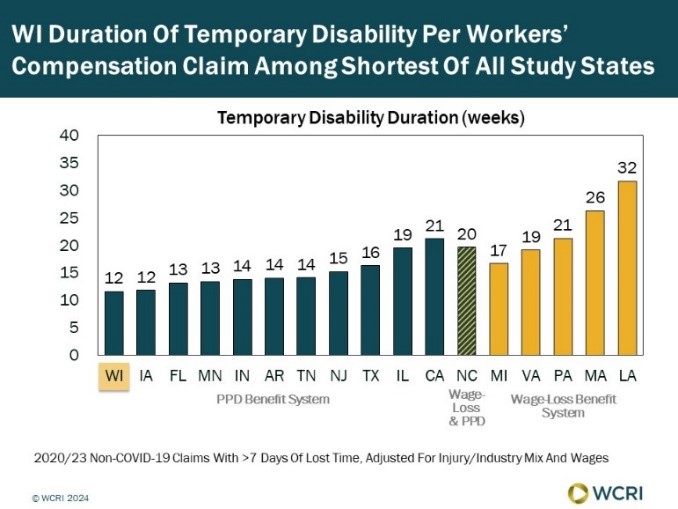

WCRI: Despite Large Growth, Wisconsin Duration of Temporary Disability per Workers’ Compensation Claim Still Shorter Than Most Study States
Waltham, MA, May 28, 2024—A recent study from the Workers Compensation Research Institute (WCRI) found that Wisconsin’s average indemnity…
-


WCRI: Hospital Outpatient Payments Lower and Growing Slower in States with Fixed-Amount Fee Schedules
Waltham, MA, May 23, 2024―With rising hospital costs a focus of public policy debates across the country, a new study from the Workers…
-
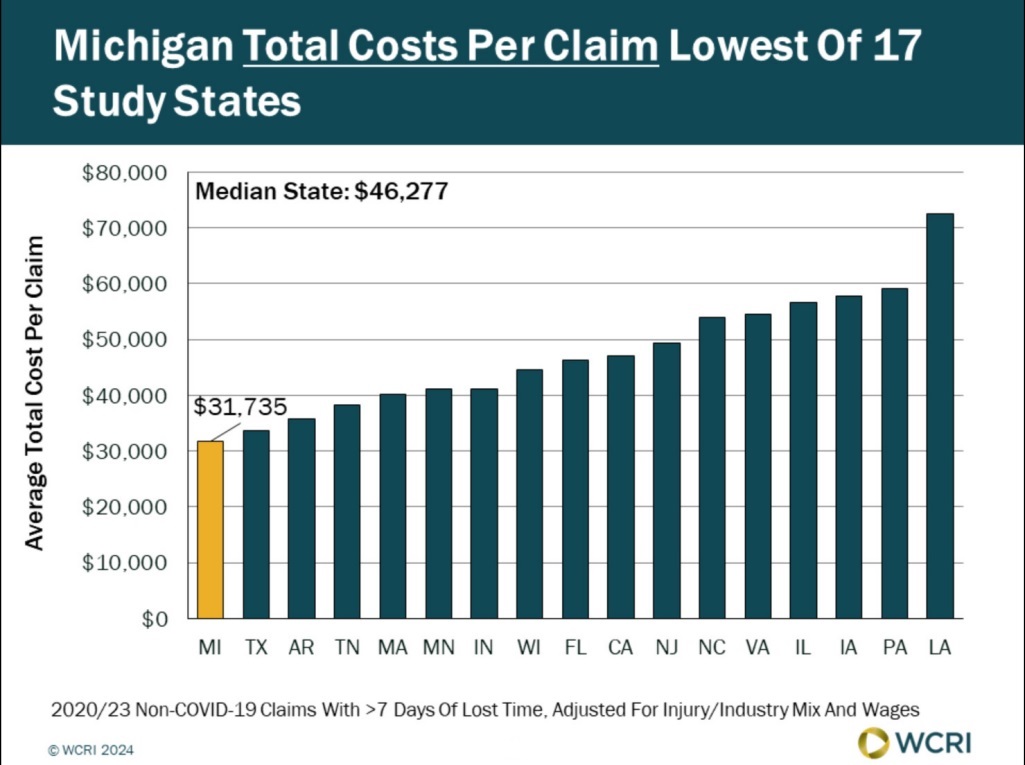

WCRI: Michigan Costs per Workers’ Compensation Claim Lowest of 17-State Study Group
Waltham, MA, May 22, 2024—A recent study from the Workers Compensation Research Institute (WCRI) found that overall costs per workers’…
-


WCRI Webinar: The Impact of Excessive Heat on Workplace Injuries
Waltham, MA, May 21, 2024—The Workers Compensation Research Institute (WCRI) will host a 30-minute webinar on Thursday, June 6, 2024, at 2 p.m.…
-
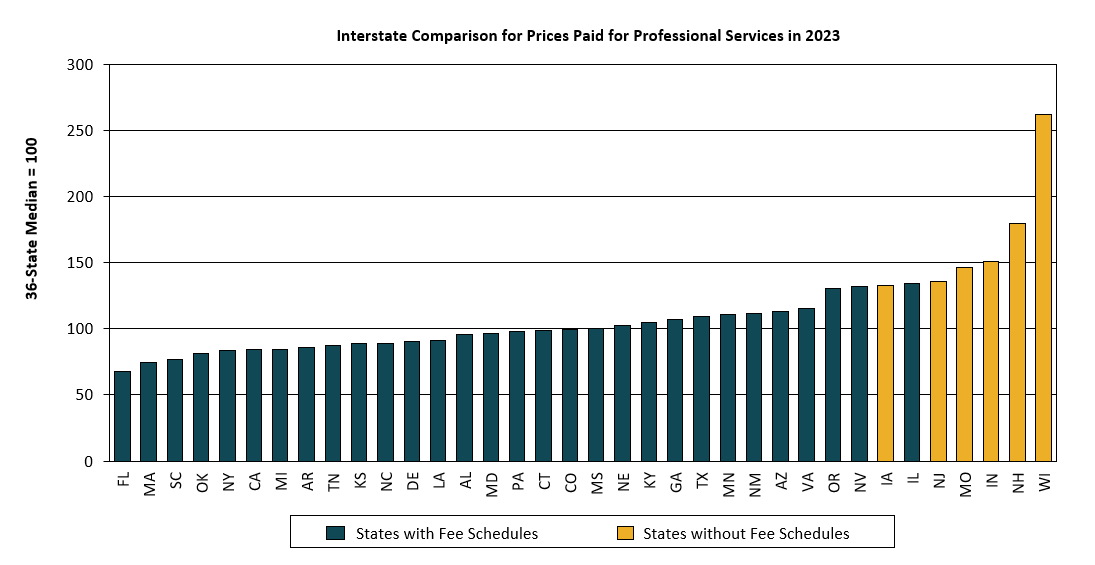

WCRI: Prices for Medical Professional Services Provided to Injured Workers Were Higher and Grew Faster in States without a Fee Schedule
Waltham, MA, May 16, 2024―Since medical costs are a constant focus for policymakers and system stakeholders in state workers’ compensation…
-
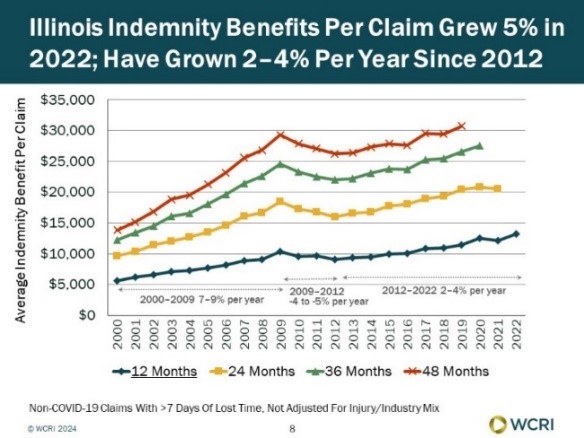

Illinois Indemnity under Workers’ Compensation Rose, but Declining Medical Payments Led to Stable Overall Costs
A new study from the Workers Compensation Research Institute (WCRI) found that indemnity benefits per claim in Illinois increased 5 percent in…
-
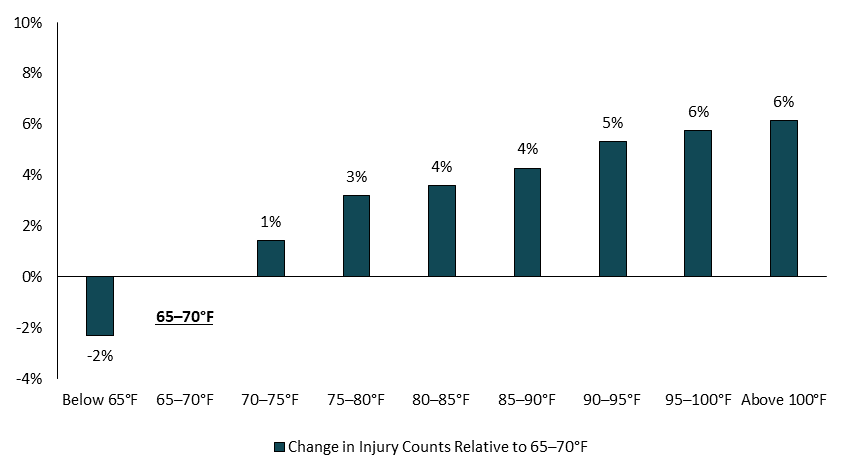

WCRI Study Explores Excessive Heat’s Influence on Workplace Injuries
Waltham, MA―With U.S. officials bracing for another summer of dangerous heat, a new study from the Workers Compensation Research Institute (WCRI)…
-
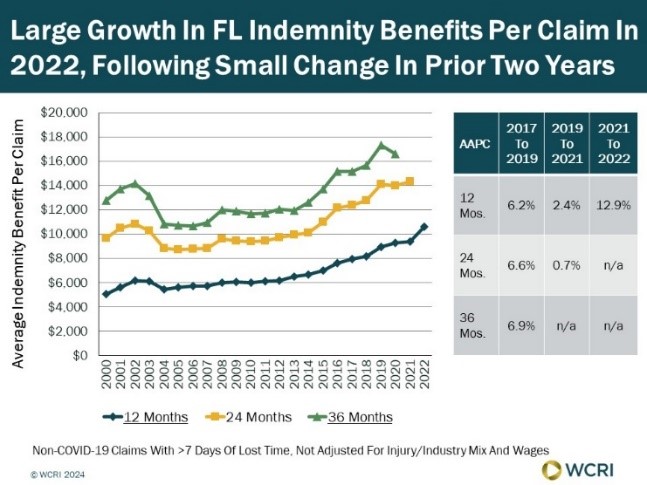

WCRI: Florida Sees Large Increase in Indemnity Benefits per Workers’ Comp Claim
A new study from the Workers Compensation Research Institute (WCRI) found that Florida’s average indemnity benefit per workers’ compensation…
-


2024 WCRI Annual Report Now Available
Waltham, MA, April 30, 2024 — The Workers Compensation Research Institute (WCRI) announced today that its 2024 WCRI Annual Report is now…
-
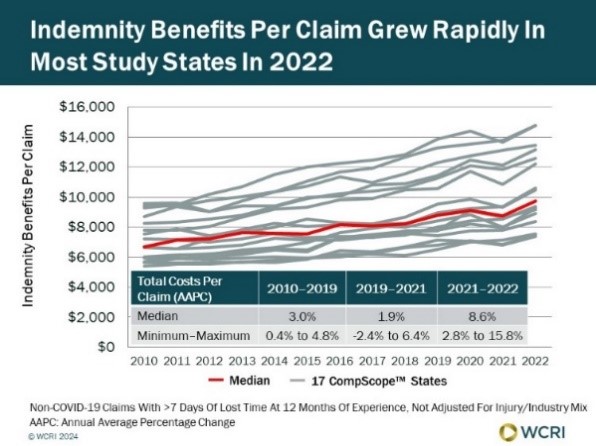

WCRI: Post-Pandemic Economic Changes Drove Rapid Increase in Indemnity Benefits for Workers’ Comp Claims in 2022
Waltham, MA, April 23, 2024―Indemnity benefits per workers’ compensation claim grew at a rapid pace of 6 percent or more in 2022 in 16 out of…
-

Webinar to Discuss Impact of Vertical Integration on Prices, Medical Utilization, and Outcomes
Waltham, MA, April 4, 2024—The Workers Compensation Research Institute (WCRI) will hold an hour-long webinar on the impact of vertical…
-


WCRI: Poorer Recovery Seen among Injured Workers with Psychosocial Risk Factors
Waltham, MA, March 28, 2024―A new study from the Workers Compensation Research Institute found that workers’ compensation patients had a higher…
-


WCRI: Tracking How State and Federal Workers’ Comp Programs Contain Medical Costs
Cambridge, MA, February 27, 2024―With medical benefits representing the single largest cost component for many state workers’ compensation…
-


Boston University Prof. Connie Noonan Hadley to Discuss the Power of Relationships to Improve Workforce Outcomes at 2024 WCRI Conference
Cambridge, MA, February 2, 2023―The Workers Compensation Research Institute (WCRI) announced today that Dr. Connie Noonan Hadley, an…
-


WCRI Conference Includes Session on Psychological Risk Factors and Functional Recovery
Cambridge, MA, Jan. 18, 2024―Today, the Workers Compensation Research Institute (WCRI) announced that a session on “Psychological Risk Factors…
-


Excessive Heat and Work-Related Injuries to Be a Focus at WCRI Conference
Cambridge, MA, Jan. 11, 2024―Today, the Workers Compensation Research Institute (WCRI) announced that a session on “Excessive Heat and…
-


WCRI: Vertical Integration Results in More Medical Care, Higher Claim Costs, and Longer Recovery after Injuries
Cambridge, MA, December 14, 2023—As vertical integration of medical providers has increased over the last decade, a new Workers Compensation…
-
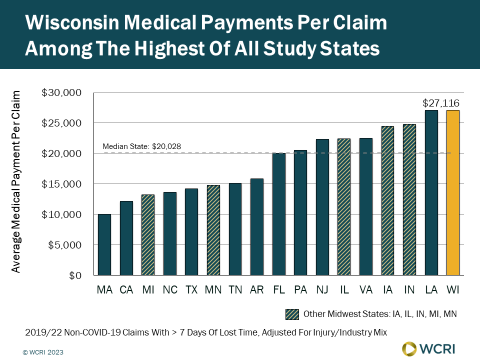

WCRI: Medical Payments for Treatment of Injured Workers in Wisconsin Highest of 17 Study States
Cambridge, MA, December 7, 2023 – A recently released study from the Workers Compensation Research Institute (WCRI) found that medical payments…
-


Time from Injury to First Medical Service among Workers’ Compensation Patients Examined before and after the Pandemic in New WCRI Study
Cambridge, MA, November 28, 2023—A new Workers Compensation Research Institute (WCRI) study, Time to First Medical Service—A WCRI FlashReport,…
-


WCRI: Mental Health Comorbidities Related to Poorer Functional Outcomes Than Physical Health Comorbidities in Workers with Low Back Pain
Cambridge, MA, November 21, 2023—A new Workers Compensation Research Institute (WCRI) study found that mental health comorbidities (anxiety,…
-
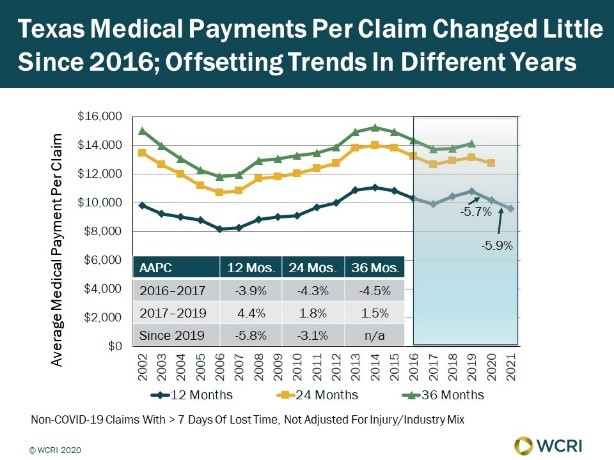

WCRI: Medical Payments to Treat Injured Workers in Texas Stable from 2016 to 2021, Masking Offsetting Trends
Cambridge, MA, November 16, 2023 – A new study from the Workers Compensation Research Institute (WCRI) found that medical payments for the…
-
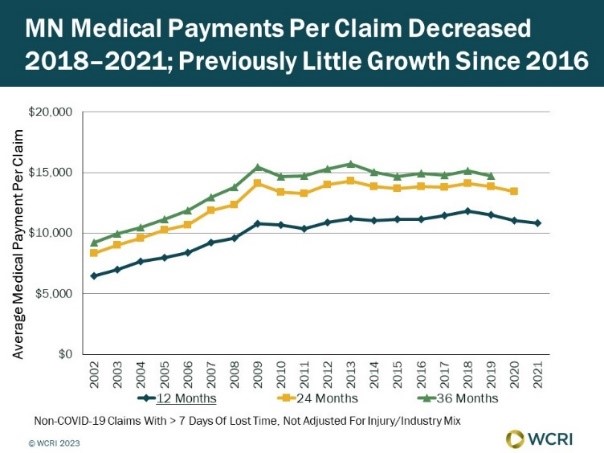

WCRI: Medical Payments for the Treatment of Injured Workers in Minnesota Continued to Decline in 2020 and 2021, Likely Due to the Pandemic
Cambridge, MA, Nov. 3, 2023 – During the first two years of the pandemic, medical payments per claim in Minnesota decreased 4 percent in…
-


WCRI Holds Webinar on CompScope™ Medical Benchmarks, 24th Edition
Cambridge, MA, Oct. 27, 2023 – The Workers Compensation Research Institute (WCRI) will hold a one-hour webinar on its recently release…
-
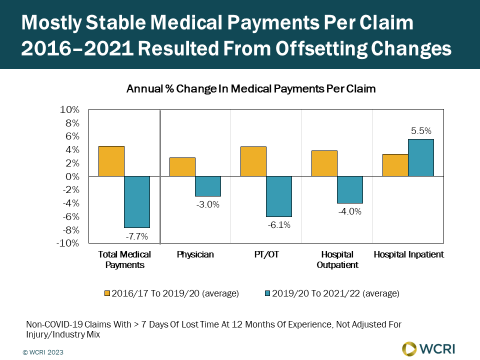

WCRI: Medical Payments for the Treatment of Injured Workers in Indiana Stable between 2016 and 2021, but Masked Offsetting Changes
Cambridge, MA, October 19, 2023 – A new study from the Workers Compensation Research Institute (WCRI) found that medical payments per workers’…
-
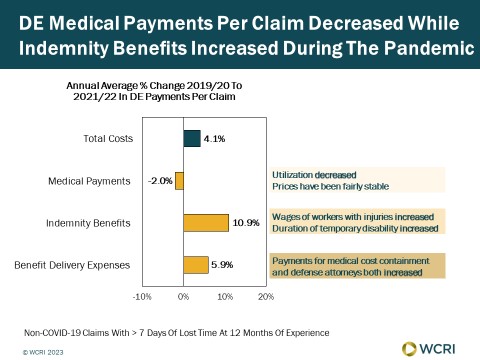

WCRI: Cost of Medical Treatment for Workers Injured on the Job in Delaware Decreased During the Pandemic, Benefit Payments Increased
Cambridge, MA, October 12, 2023 — A new study from the Workers Compensation Research Institute (WCRI) found that total costs per claim with more…
-


2024 WCRI Conference: Keynote Announced and Registration Open
Cambridge, MA, Oct. 10, 2023―The Workers Compensation Research Institute (WCRI) announced today that registration is open and acclaimed Harvard…
-
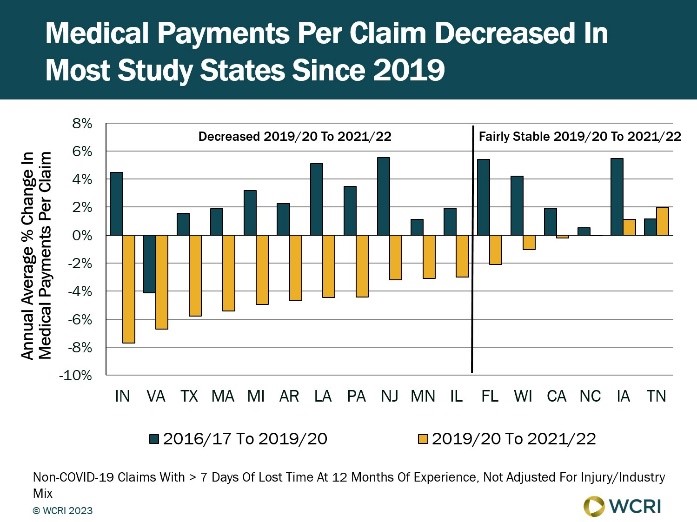

WCRI: Medical Payments Continued to Decline in 2021, Reflecting Lingering Effects of Pandemic
Cambridge, MA, October 5, 2023 ― Medical payments per claim decreased more than 3 percent in most of the 17 study states for 2021 injuries with…
-


WCRI Holds Webinar on Long COVID in the Workers’ Compensation System in 2020 and 2021
Cambridge, MA, Sept. 15, 2023 – The Workers Compensation Research Institute (WCRI) will hold a 30-min. webinar on its study Long COVID in the…
-


WCRI Study Examines Impact of Workforce Changes on Workers’ Compensation Outcomes
Cambridge, MA, August 31, 2023 – A new study from the Workers Compensation Research Institute (WCRI) found the recent economic trends and the…
-


WCRI: Long COVID Affected 6 Percent of Workers with COVID-19 Claims in 2020 and 2021
Cambridge, MA, August 17, 2023 – A new study from the Workers Compensation Research Institute (WCRI) found that 6 percent of workers with…
-


WCRI Webinar on Medical Inflation in Workers’ Compensation
Join the Workers Compensation Research Institute (WCRI) for a 30-min. webinar on Wed., Sept. 6, 2023, at 2:00 pm ET as authors Olesya Fomenko and…
-


WCRI: No Evidence of a Steep Medical Price Growth in Workers’ Compensation during the Recent Inflationary Period
Cambridge, MA, August 3, 2023 – The steep growth in consumer prices for energy, food, and housing over the last few years created concerns about…
-
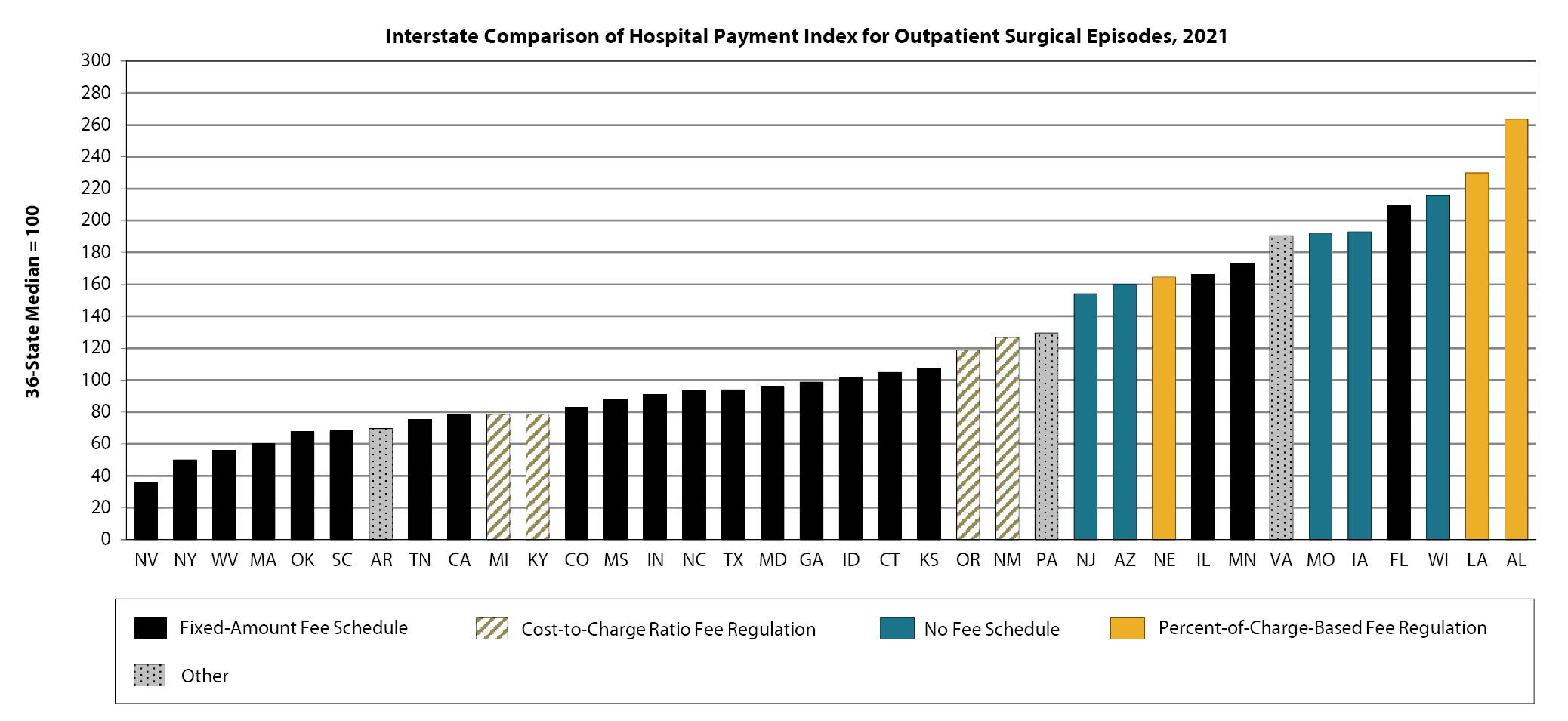

WCRI: Hospital Outpatient Payments Lower and Growing Slower in States with Fixed-Amount Fee Schedules
Cambridge, MA, May 31, 2023 – During these times when rising hospital costs are a focus of public policy debates, a new study from the Workers…
-
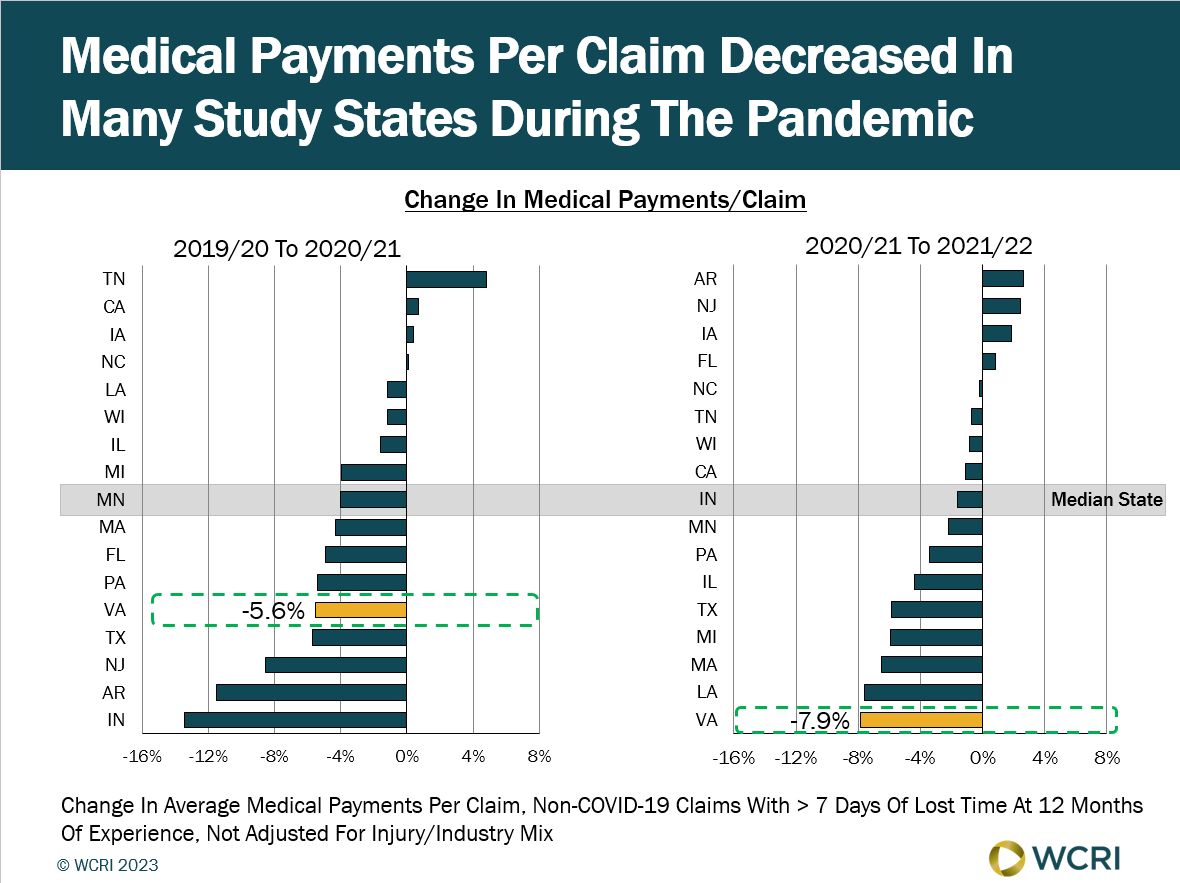

WCRI: Pandemic May Have Played Role in Decrease of Medical Payments per Workers’ Compensation Claim in Virginia
Cambridge, MA, May 30, 2023 – Medical payments per workers' compensation claim in Virginia at 12 months of maturity decreased 5.6 percent…
-
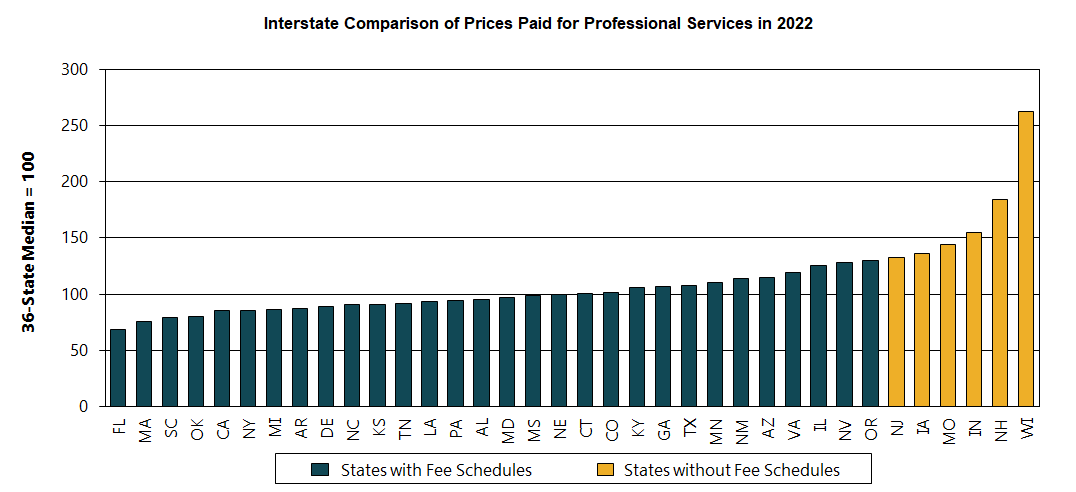

WCRI: Substantial Variation Found in Prices Paid for Professional Medical Services to Treat Injured Workers in 36 States
Cambridge, MA, May 18, 2023 ― Today, the Workers Compensation Research Institute (WCRI) released an updated version of its study that compares…
-
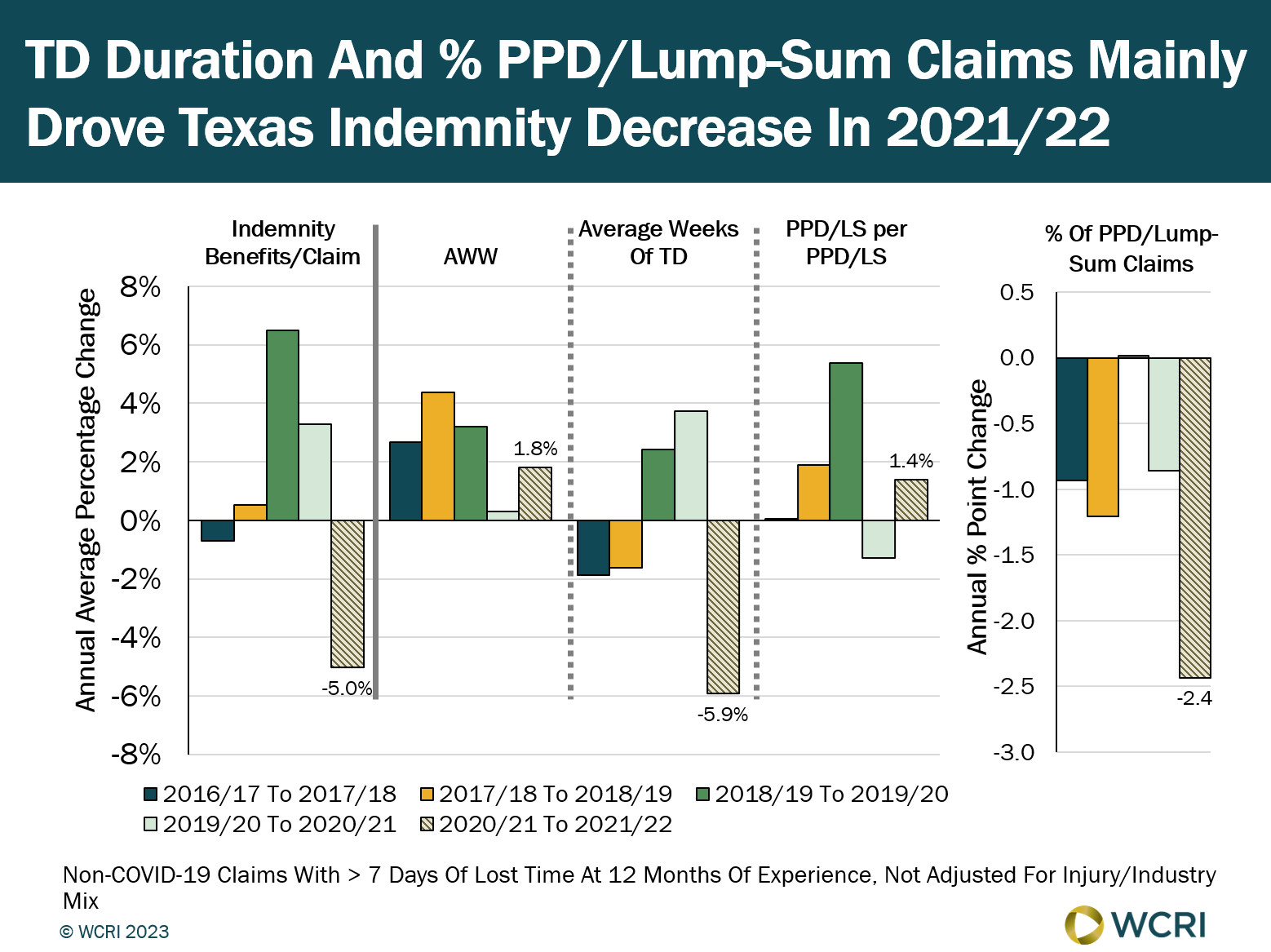

WCRI: Changes in Texas Duration of Temporary Disability May Relate to COVID-19 Pandemic
Cambridge, MA, May 16, 2023 – Trends in indemnity components in Texas differed between 2016 and 2021, though wages of workers with injuries grew…
-
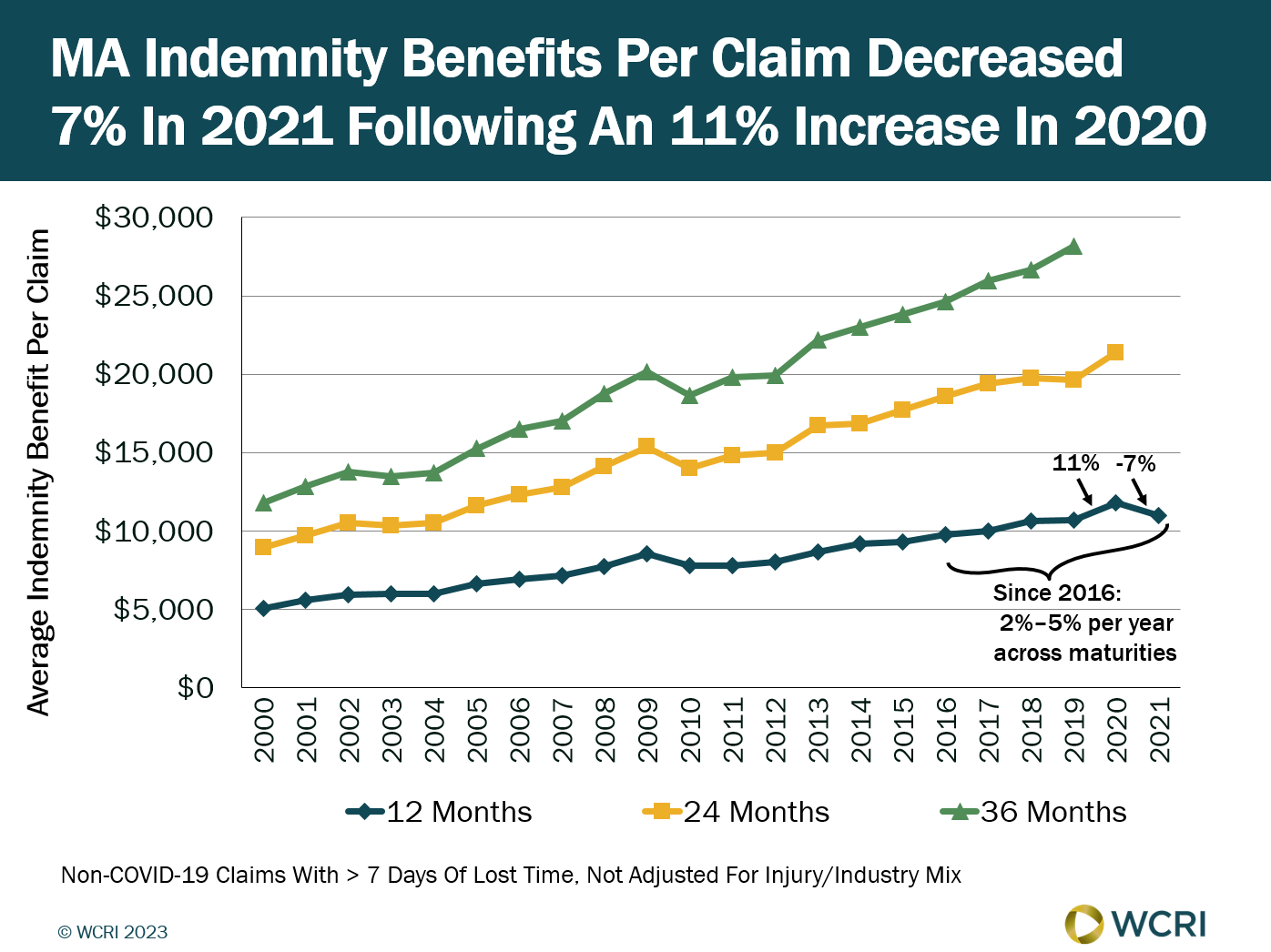

WCRI: COVID-19 Pandemic Likely Contributed to the Trends in Indemnity Benefits in Massachusetts
Cambridge, MA, May 9, 2023 – Indemnity benefits per claim in Massachusetts decreased 7 percent in 2021 following a sizeable increase in the…
-
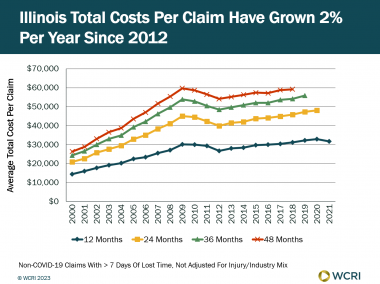

WCRI: Total Costs per Workers’ Compensation Claim in Illinois Changed Little during the Pandemic
Cambridge, MA, May 2, 2023 – The average total cost per claim in Illinois changed little between 2019 and 2021 for injuries evaluated as of the…
-


2023 WCRI Annual Report Now Available
Cambridge, MA, April 27, 2023 – The Workers Compensation Research Institute (WCRI) announced today that its 2023 WCRI Annual Report is now…
-


WCRI: Florida Costs per Claim Remained Stable in the First Two Years of COVID-19 Pandemic
Cambridge, MA, April 25, 2023—Total costs per claim with more than seven days of lost time in Florida remained stable in 2020 and 2021, following…
-
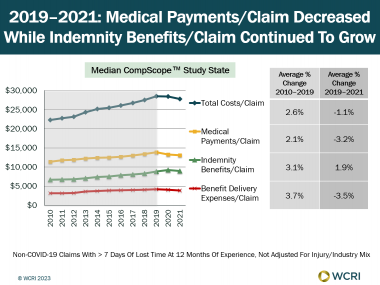

WCRI: COVID-19 Pandemic Continues to Impact Indemnity Benefits and Medical Payments in Various States
Cambridge, MA, April 18, 2023 – A new series of 14 studies from the Workers Compensation Research Institute (WCRI) found medical payments per…
-


WCRI Releases National Inventory of State Regulations Affecting Prescription Drugs
Cambridge, MA, April 4, 2023―Today, the Workers Compensation Research Institute (WCRI) released a new report that gathers in one place the…
-


Ramona Tanabe to Succeed John Ruser as New WCRI CEO
Cambridge, MA, April 3, 2023―The Workers Compensation Research Institute (WCRI) announced today that executive vice president Ramona Tanabe has…
-


New WCRI Studies Monitor the Impact of Drug Formularies
Cambridge, MA, March 30, 2023―A series of studies from the Workers Compensation Research Institute (WCRI) examines the impact of formularies on…
-


New WCRI Study Compares Physicians’ Involvement in the Workers’ Compensation System across 34 States
Cambridge, MA, March 28, 2023―A new study from the Workers Compensation Research Institute (WCRI) helps policymakers and stakeholders get an…
-
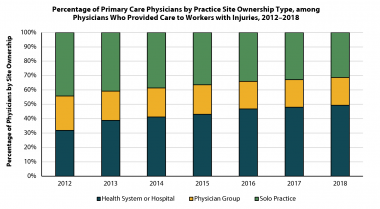

WCRI: Costs to Treat Injured Workers Increase 8 Percent after Physician Practices Are Acquired by Hospitals
Cambridge, MA, March 16, 2023―A new study from the Workers Compensation Research Institute (WCRI) examines the impact of vertical integration of…
-


Panel to Discuss the Impact of the Labor Shortage at 2023 WCRI Conference
Cambridge, MA, March 2, 2023― Today, the Workers Compensation Research Institute (WCRI) shared information about a panel on the “Impact of the…
-
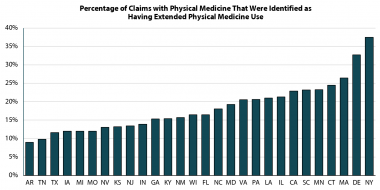

WCRI Identifies Factors Associated with Extended Use of Physical Medicine Services
Cambridge, MA, March 1, 2023―Extended physical medicine (PM) use was relatively frequent in most study states and less coordination of care was…
